Arrive
Birth Matters: January 2020
By Laura Maxson LM
When parents think about the words baby and arrive they are generally thinking about when labor is going to start. But for more and more families, labor is not going to start on its own – it’s going to begin with an induction of labor.
All thanks to the recent ARRIVE study, Labor Induction versus Expectant Management in Low-Risk Nulliparous Women, which looks at inducing otherwise healthy pregnancies at 39 weeks.
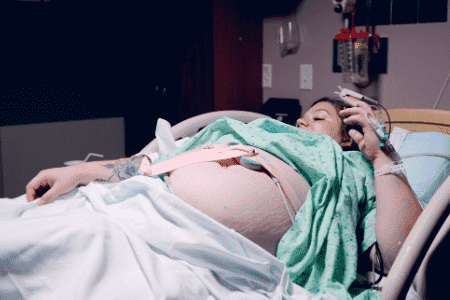
Some are interpreting the results as a reason for routine induction of labor at 39 weeks for everyone. “Our data suggest that 1 cesarean delivery may be avoided for every 28 deliveries among low-risk nulliparous women [someone who has never given birth to a live baby] who plan to undergo elective induction of labor at 39 weeks.”
Forty-one different clinical locations, with a variety of induction methods were used in the study of 6000 births, with only 6% of those births attended by midwives. Induction medicalizes birth with hospital beds often occupied for many days. This may raise maternity costs, as well as change the feel of birth from a life event to a medical procedure. Spontaneous labors generally unfold with early labor spent at home before going to the hospital in active labor.
In response to the study, ACOG (American College of Obstetricians and Gynecologists) reminds care providers “…that this recommendation may be conditional upon the values and preferences of the pregnant woman.” And the California Maternal Quality Care Collaborative states, “Specifically, induction of labor at less than 41 weeks 0 days with an unfavorable cervix should only be performed for medical indications.” Even so, parents can be made to feel that they are endangering their child by opting out of routine induction.
When the standard of care tips in favor of routine induction of labor, prenatal visits may begin to focus on induction information instead of planning for a spontaneous birth. It is not uncommon for it to take 2-3 days to get labor started with induction. This is very different in comparison with continuing to work or puttering around at home waiting for labor to begin. Those last weeks of pregnancy can be an important part of becoming ready to become a parent.
Induction of labor can include:
Folley bulb. An inflatable catheter is inserted through a slightly open cervix. The catheter is then inflated between the bag of waters and the cervix, applying pressure to help dilate the cervix.
Rupturing the membranes. Breaking the bag of waters is often performed as part of an induction.
Cervical ripening drugs such as Misoprostol. This drug, often referred to as “Miso”, can be given orally or placed vaginally to ripen the cervix and/or begin contractions. While effective, it can cause hard and strong labor leaving many women shaken or slammed by unrelenting contractions.

Pitocin. Oxytocin (brand name Pitocin) is given via IV to stimulate contractions. While essentially the same hormone that the body produces to make contractions, it is only delivered into the bloodstream via IV. Natural production of oxytocin on the other hand, is released into the brain as well as the bloodstream stimulating the release of natural endorphins to help cope with labor.
The use of Pitocin leads to epidurals for many women. Pitocin and epidural use will require continuous electronic fetal monitoring, as both can cause the baby to become distressed. Days of IV fluids from Pitocin and epidurals can lead to fluid retention, which in turn, can lead to challenges with breastfeeding. Breastfeeding was not addressed in the study.
As families begin to feel the effects of the ARRIVE study, intended to reduce cesareans, many wonder why other cesarean reduction techniques are not adopted. Routine electronic fetal monitoring in low risk labors, increases cesareans. While there is some movement to adopt intermittent auscultation (using a fetal Doppler to listen to the baby instead) it is still somewhat rare.
Midwifery care decreases cesareans. Nationwide, fewer than 9% of all pregnancies are attended by hospital midwives. While all three of Santa Cruz County’s hospitals offer midwife deliveries, an increase in midwifery deliveries should help decrease cesareans. In 2018 licensed homebirth midwives in California had a 7% cesarean rate. Yet, OBs rarely encouraged families to consider homebirth. No matter what the ARRIVE study may say about reducing cesareans, a primary cesarean rate of 18% for low-risk pregnancies is triple the overall cesarean rate of 5.5% in the 1970s and is still way too high.
Methods of Induction – aafp.org/afp/2003/0515/p2123.html
2018 Licensed Midwife Report – https://www.mbc.ca.gov/Licensees/Midwives/
Birth Network of Santa Cruz County – www.birthnet.org
Laura Maxson has been the director of Birth Network since 1998. She became an advocate in the early ’80s after experiencing a lack of information and choice around birth and breastfeeding. Laura has worked as a breastfeeding counselor, childbirth educator, doula, and homebirth midwife.






