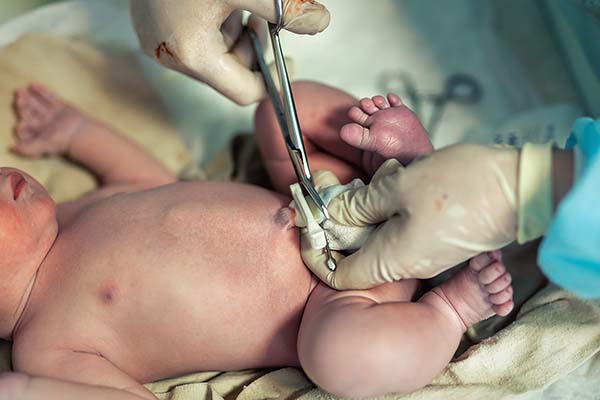
Optimal Cord Clamping
BY Laura Maxson, LM

Mothers of animals born with intact cords are focused intently on their babies – sniffing, licking (kissing), and nuzzling – stimulating them to breathe and bond.
Before birth the placenta does the baby’s breathing (gas exchange), so the lungs are resting and essentially bypassed by blood circulation. The lungs are made up of fluid-filled air sacs surrounded by tiny blood vessels that are tightly constricted due to lack of blood flow. After birth, as the baby begins to breathe, blood circulation changes dramatically and rushes to the lungs as these tiny vessels relax and swell with blood to begin working.
This means that beginning to breathe takes lots of blood. Ideally, the blood that rushes to help open the lungs comes from the placenta as an addition to the baby’s circulation if the cord is still intact But, when the cord has already been cut the “extra” blood to help open the lungs must be redistributed from the baby’s system. Organs, including the brain, can be robbed of vital blood supply.
Nature provides a supported transition to breathing by continuing to provide oxygenated blood for several minutes after birth through the placenta and intact cord. Mothers of animals born with intact cords are focused intently on their babies – sniffing, licking (kissing), and nuzzling – stimulating them to breathe and bond. Animal mothers generally don’t fiddle with the cord until much later, when their baby is breathing and the cord is limp, empty, and finished pulsing.
Cord Management of theTerm Newborn, 2 August 2021, Ola Andersson, PhD, MD and Judith S. Mercer, PhD, CNM, provides new information on the value and timing of delaying cord clamping, suggesting at least three minutes after birth before clamping the cord and not to depend on the end of pulsations. The American College of Nurse–Midwives recommends delayed umbilical cord clamping for term and preterm infants for 2–5 minutes after birth. The American College of Obstetricians and Gynecologists (ACOG) only recommends a delay in umbilical cord clamping in vigorous term and preterm infants for at least 30–60 seconds, seemingly ignoring the benefits of a more complete transfer of a few more ounces of blood to the baby, which also increases plasma, red blood cells, several million to a billion stem cells, and more. In a full term infant, this provides iron stores for the first 3 to 8 months. In a preemie, it helps prevent intraventricular hemorrhage (brain bleed), sepsis (infection), and necrotizing enterocolitis. The increased myelination of nerve cells helps in early brain development, as well as fine motor development and increased social skills at 4 years of age. (link below for more information.)
Changing the timing of cord clamping means changing habits and protocols. Because one care provider is generally responsible for the care of the mother and another for the baby, cutting the cord has represented a clear handoff of responsibility. Most obstetrical training includes early cord clamping as part of managing delivery of the placenta. Pediatricians and nursery staff, often trained to evaluate a newborn baby immediately after birth on a heated baby bed across the room, have moved to assessment with baby skin-to-skin. However, babies most in need of delayed cord clamping – those who need help to begin breathing – are the ones most likely to have the quickest clamping to move to the resuscitation area.
Homebirth midwives value the intact cord during the newborn’s transition (especially during resuscitation) and, being responsible for both mother and baby, can easily tailor their responses to the immediate needs of the situation. Because the hospital’s resuscitation equipment is often contained in the baby bed across the room, resuscitation often can’t begin without the cord being cut, essentially cutting off the available oxygenated blood readily supplied by the placenta, at the time it is needed the most.
Thankfully, we are beginning to see more opportunities for optimal cord clamping. Many babies go straight into mother’s arms for initial assessment instead of off to the baby warmer across the room. But it is far from routine for all providers or for all circumstances to agree to 5 minutes or more before clamping the cord, often using the now essentially debunked risk of complications from jaundice as the reasoning.
Changes in mindset and logistics stand in the way of optimal cord clamping in the hospital. Investment in bedside baby trolleys that allow resuscitation with the cord intact is needed, along with the willingness of practitioners to adjust to helping babies breathe at bedside. Real change begins with parents asking for a delay in clamping the cord for at least 5 minutes and discussing considering keeping the cord intact if resuscitation efforts are necessary.
Cord Management of the Term Newborn: sciencedirect.com/science/article/pii/S0095510821000415
Midwives, Doulas & Childbirth Educators – birthnet.org
Laura Maxson has been the director of Birth Network since 1998. She became an advocate in the early ’80s after experiencing a lack of information and choice around birth and breastfeeding. Laura has worked as a breastfeeding counselor, childbirth educator, doula, and homebirth midwife.